REGIONAL and rural medical students will have the opportunity to remain in regional areas to complete specialist training thanks to the establishment of a regional training hub.
Subscribe now for unlimited access.
$0/
(min cost $0)
or signup to continue reading
The hub, which will encompass UNSW Rural Clinical Schools in Albury, Wagga and Port Macquarie, will be one of 26 across the country under the federal government's Rural Health Multidisciplinary Training program.
Albury head of campus Dr Neil Bright said the hub would help regional areas retain young doctors.
“The idea behind the training hubs is that co-ordinate training with colleges and hospitals so that young medical graduates can do their intern years and continue on into surgical, medical, anaesthetic or pathology training and spend the majority of their time in rural and regional Australia,” he said.
“That would likely increase the retention rate of doctors.
“At the moment we're sending people to Melbourne or Sydney at a time in their lives where they're more likely to form relationships, start mortgages, start families.
“Once they've done that, it's very difficult to get them to leave and come back.
“A large percentage of students look at moving back to capital cities because they're worried that they won't get into the specialist training programs they want to.
“It's imperative that we have this training hub in the long term because without it, we are not going to get people to stay and grow the great services we have here.”
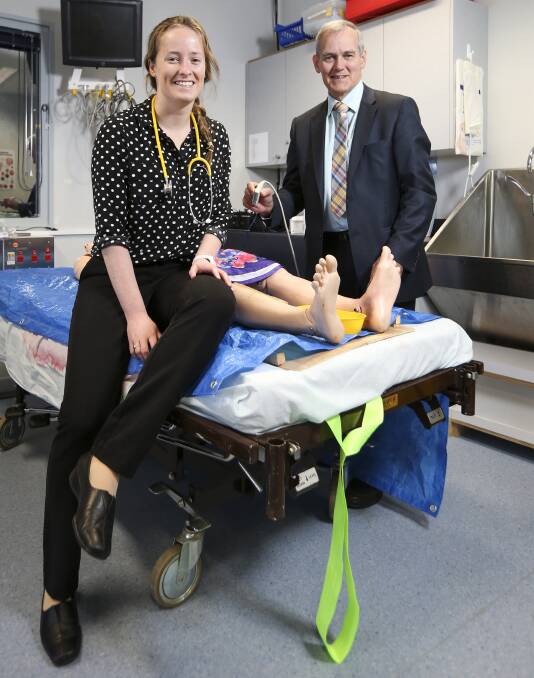
UNSW student Katherine Grellman said having the chance to complete her studies and transition directly into specialist training was important to her.
“For some of us who have spent the last four years here, it means we don’t have to uproot and do a couple of years in Sydney or Melbourne before coming back to do the specialist training we want to do,” she said.
“The financial cost of moving is one thing, but we've all lived here for a while now, become part of the community.”
Dr Bright said keeping young doctors in regional areas would also reduce the likelihood of shortages in speciality areas.
“If you look around here there are only two ear, nose and throat surgeons,” he said.
“If one got sick the service would be in serious trouble.
“If we're growing our own people here, it makes a huge difference.”


